Business Name: BeeHive Homes of Hitchcock
Address: 6714 Delany Rd, Hitchcock, TX 77563
Phone: (409) 800-4233
BeeHive Homes of Hitchcock
For people who no longer want to live alone, but aren't ready for a Nursing Home, we provide an alternative. A big assisted living home with lots of room and lots of LOVE!
6714 Delany Rd, Hitchcock, TX 77563
Business Hours
Monday thru Saturday: Open 24 hours
Facebook: https://www.facebook.com/bhhohitchcock
Families seldom get to memory care after a single conversation. It generally follows months or years of small losses that build up: the stove left on, a mix-up with medications, a familiar community that unexpectedly feels foreign to somebody who liked its regimen. Alzheimer's changes the way the brain processes info, however it does not erase a person's need for dignity, significance, and safe connection. The best memory care programs comprehend this, and they build daily life around what remains possible.
I have actually walked with households through evaluations, move-ins, and the irregular middle stretch where development appears like fewer crises and more excellent days. What follows comes from that lived experience, shaped by what caregivers, clinicians, and residents teach me daily.
What "lifestyle" means when memory changes
Quality of life is not a single metric. With Alzheimer's, it usually includes five threads: security, comfort, autonomy, social connection, and purpose. Security matters since roaming, falls, or medication mistakes can change whatever in an instant. Convenience matters due to the fact that agitation, discomfort, and sensory overload can ripple through an entire day. Autonomy protects dignity, even if it implies choosing a red sweater over a blue one or choosing when to sit in the garden. Social connection reduces isolation and frequently improves appetite and sleep. Purpose might look various than it utilized to, however setting the tables for lunch or watering herbs can offer somebody a reason to stand and move.
Memory care programs are created to keep those threads undamaged as cognition modifications. That style appears in the hallways, the staffing mix, the daily rhythm, and the method personnel method a resident in the middle of a challenging moment.
Assisted living, memory care, and where the lines intersect
When households ask whether assisted living suffices or if dedicated memory care is needed, I normally start with an easy concern: Just how much cueing and guidance does your loved one need to survive a normal day without risk?
Assisted living works well for elders who need help with day-to-day activities like bathing, dressing, or meals, but who can dependably browse their environment with periodic assistance. Memory care is a specific type of assisted living developed for individuals with Alzheimer's or other dementias who benefit from 24-hour oversight, structured regimens, and personnel trained in behavioral and communication techniques. The physical environment varies, too. You tend to see secured yards, color hints for wayfinding, reduced visual clutter, and typical areas established in smaller, calmer "communities." Those features decrease disorientation and assistance residents move more freely without consistent redirection.
The option is not just scientific, it is practical. If wandering, duplicated night wakings, or paranoid deceptions are appearing, a conventional assisted living setting might not have the ability to keep your loved one engaged and safe. Memory care's customized staffing ratios and programming can capture those problems early and respond in manner ins which lower tension for everyone.
The environment that supports remembering
Design is not decoration. In memory care, the built environment is among the primary caretakers. I have actually seen citizens discover their spaces dependably due to the fact that a shadow box outside each door holds pictures and little keepsakes from their life, which end up being anchors when numbers and names slip away. High-contrast plates can make food easier to see and, surprisingly often, improve intake for somebody who has been eating improperly. Great programs manage lighting to soften night shadows, which assists some residents who experience sundowning feel less nervous as the day closes.
Noise control is another peaceful victory. Instead of tvs blaring in every common room, you see smaller areas where a few individuals can check out or listen to music. Overhead paging is rare. Floors feel more residential than institutional. The cumulative result is a lower physiological tension load, which typically equates to fewer habits that challenge care.
Routines that lower anxiety without taking choice
Predictable structure helps a brain that no longer processes novelty well. A normal day in memory care tends to follow a mild arc. Morning care, breakfast, a brief stretch or walk, an activity block, lunch, a pause, more shows, dinner, and a quieter evening. The information differ, but the rhythm matters.
Within that rhythm, choice still matters. If somebody invested mornings in their garden for forty years, a good memory care program finds a method to keep that routine alive. It may be a raised planter box by a warm window or an arranged walk to the courtyard with a little watering can. If a resident was a night owl, requiring a 7 a.m. wake time can backfire. The best groups learn everyone's story and utilize it to craft routines that feel familiar.
I visited a neighborhood where a retired nurse awakened distressed most days till personnel provided her an easy clipboard with the "shift projects" for the early morning. None of it was genuine charting, however the small role restored her sense of proficiency. Her stress and anxiety faded because the day lined up with an identity she still held.
Staff training that changes hard moments
Experience and training different typical memory care from excellent memory care. Strategies like recognition, redirection, and cueing may seem like jargon, but in practice they can transform a crisis into a workable moment.
A resident demanding "going home" at 5 p.m. may be trying to return to a memory of safety, not an address. Remedying her often intensifies distress. An experienced caretaker may validate the feeling, then use a transitional activity that matches the requirement for movement and purpose. "Let's check the mail and then we can call your daughter." After a short walk, the mail is checked, and the worried energy dissipates. The caregiver did not argue realities, they fulfilled the emotion and rerouted gently.
Staff also discover to spot early indications of discomfort or infection that masquerade as agitation. An unexpected rise in uneasyness or rejection to eat can indicate a urinary system infection or constipation. Keeping a low-threshold procedure for medical assessment prevents small concerns from becoming health center sees, which can be deeply disorienting for someone with dementia.
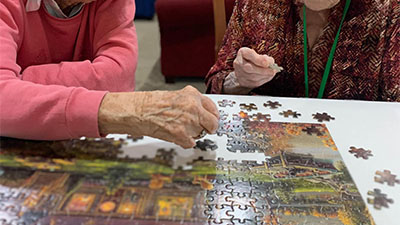
Activity style that fits the brain's sweet spot
Activities in memory care are not busywork. They aim to promote preserved capabilities without overloading the brain. The sweet area varies by person and by hour. Great motor crafts at 10 a.m. may be successful where they would annoy at 4 p.m. Music invariably shows its worth. When language fails, rhythm and tune often remain. I have actually viewed someone who seldom spoke sing a Sinatra chorus in ideal time, then smile at a staff member with acknowledgment that speech might not summon.
Physical motion matters simply as much. Brief, supervised strolls, chair yoga, light resistance bands, or dance-based workout lower fall threat and aid sleep. Dual-task activities, like tossing a beach ball while calling out colors, combine motion and cognition in a way that holds attention.

Sensory engagement works for citizens with advanced disease. Tactile materials, aromatherapy with familiar fragrances like lemon or lavender, and calm, repetitive assisted living BeeHive Homes of Hitchcock tasks such as folding hand towels can regulate nerve systems. The success procedure is not the folded towel, it is the unwinded shoulders and the slower breathing that follow.
Nutrition, hydration, and the little tweaks that add up
Alzheimer's impacts cravings and swallowing patterns. Individuals might forget to consume, fail to recognize food, or tire quickly at meals. Memory care programs compensate with a number of strategies. Finger foods help residents keep self-reliance without the obstacle of utensils. Offering smaller, more frequent meals and snacks can increase total intake. Brilliant plateware and uncluttered tables clarify what is edible and what is not.
Hydration is a peaceful fight. I prefer noticeable hydration hints like fruit-infused water stations and personnel who use fluids at every shift, not just at meals. Some neighborhoods track "cup counts" informally throughout the day, capturing down trends early. A resident who consumes well at room temperature may prevent cold drinks, and those preferences ought to be documented so any team member can step in and succeed.
Malnutrition shows up discreetly: looser clothing, more daytime sleep, an uptick in infections. Dietitians can change menus to add calorie-dense options like smoothies or prepared soups. I have actually seen weight stabilize with something as easy as a late-afternoon milkshake ritual that locals anticipated and really consumed.
Managing medications without letting them run the show
Medication can assist, but it is not a remedy, and more is not always much better. Cholinesterase inhibitors and memantine provide modest cognitive benefits for some. Antidepressants may reduce stress and anxiety or enhance sleep. Antipsychotics, when used moderately and for clear indications such as consistent hallucinations with distress or extreme aggression, can soothe harmful circumstances, but they bring threats, consisting of increased stroke threat and sedation. Excellent memory care teams work together with physicians to evaluate medication lists quarterly, taper where possible, and favor nonpharmacologic methods first.
One useful secure: a comprehensive evaluation after any hospitalization. Medical facility remains typically include new medications, and some, such as strong anticholinergics, can aggravate confusion. A devoted "med rec" within 2 days of return saves numerous residents from avoidable setbacks.
Safety that feels like freedom
Secured doors and roam management systems lower elopement danger, however the objective is not to lock individuals down. The goal is to enable motion without constant worry. I look for communities with secure outside spaces, smooth pathways without journey risks, benches in the shade, and garden beds at standing and seated heights. Strolling outdoors lowers agitation and enhances sleep for lots of citizens, and it turns security into something suitable with joy.
Inside, inconspicuous innovation supports independence: movement sensors that trigger lights in the bathroom in the evening, pressure mats that signal staff if somebody at high fall risk gets up, and discreet cams in corridors to keep an eye on patterns, not to invade personal privacy. The human part still matters most, but smart design keeps citizens much safer without advising them of their restrictions at every turn.
How respite care suits the picture
Families who offer care in the house typically reach a point where they need short-term help. Respite care gives the person with Alzheimer's a trial remain in memory care or assisted living, usually for a couple of days to several weeks, while the primary caretaker rests, takes a trip, or manages other obligations. Great programs treat respite locals like any other member of the community, with a customized strategy, activity involvement, and medical oversight as needed.
I motivate families to use respite early, not as a last resort. It lets the staff learn your loved one's rhythms before a crisis. It likewise lets you see how your loved one reacts to group dining, structured activities, and a different sleep environment. Often, families find that the resident is calmer with outside structure, which can notify the timing of an irreversible move. Other times, respite supplies a reset so home caregiving can continue more sustainably.
Measuring what "much better" looks like
Quality of life enhancements appear in regular locations. Fewer 2 a.m. telephone call. Less emergency clinic sees. A steadier weight on the chart. Less tearful days for the spouse who used to be on call 24 hr. Personnel who can inform you what made your father smile today without examining a list.
Programs can quantify a few of this. Falls monthly, healthcare facility transfers per quarter, weight patterns, participation rates in activities, and caretaker complete satisfaction surveys. However numbers do not inform the entire story. I look for narrative documents also. Development notes that state, "E. joined the sing-along, tapped his foot to 'Blue Moon,' and stayed for coffee," assistance track the throughline of somebody's days.
Family participation that reinforces the team
Family sees stay vital, even when names slip. Bring existing photos and a few older ones from the era your loved one remembers most plainly. Label them on the back so staff can utilize them for conversation. Share the life story in concrete details: favorite breakfast, tasks held, crucial animals, the name of a lifelong pal. These end up being the raw products for meaningful engagement.
Short, predictable gos to frequently work much better than long, tiring ones. If your loved one becomes nervous when you leave, a personnel "handoff" helps. Agree on a little routine like a cup of tea on the patio, then let a caretaker transition your loved one to the next activity while you slip out. With time, the pattern reduces the distress peak.
The expenses, trade-offs, and how to examine programs
Memory care is costly. In numerous regions, month-to-month rates run higher than traditional assisted living since of staffing ratios and specialized shows. The cost structure can be complex: base rent plus care levels, medication management, and secondary services. Insurance coverage is restricted; long-term care policies sometimes help, and Medicaid waivers might use in specific states, typically with waitlists. Families need to prepare for the monetary trajectory honestly, including what occurs if resources dip.
Visits matter more than sales brochures. Drop in at different times of day. Notice whether citizens are engaged or parked by televisions. Smell the location. Watch a mealtime. Ask how staff deal with a resident who withstands bathing, how they interact changes to households, and how they handle end-of-life transitions if hospice becomes proper. Listen for plainspoken answers instead of polished slogans.
A simple, five-point walking checklist can hone your observations during tours:
- Do staff call homeowners by name and method from the front, at eye level? Are activities taking place, and do they match what locals in fact appear to enjoy? Are hallways and spaces without mess, with clear visual hints for navigation? Is there a safe outdoor area that residents actively use? Can leadership explain how they train brand-new personnel and keep experienced ones?
If a program balks at those questions, probe further. If they answer with examples and welcome you to observe, that confidence generally reflects genuine practice.
When habits challenge care
Not every day will be smooth, even in the best setting. Alzheimer's can bring hallucinations, sleep reversal, fear, or refusal to bathe. Efficient teams begin with triggers: discomfort, infection, overstimulation, irregularity, appetite, or dehydration. They change routines and environments first, then consider targeted medications.
One resident I knew started shouting in the late afternoon. Staff noticed the pattern aligned with household gos to that stayed too long and pushed previous his fatigue. By moving sees to late morning and using a brief, peaceful sensory activity at 4 p.m. with dimmer lights, the shouting almost disappeared. No brand-new medication was needed, simply various timing and a calmer setting.
End-of-life care within memory care
Alzheimer's is a terminal disease. The last phase brings less mobility, increased infections, trouble swallowing, and more sleep. Excellent memory care programs partner with hospice to handle signs, line up with household goals, and safeguard comfort. This stage frequently requires fewer group activities and more concentrate on gentle touch, familiar music, and pain control. Households gain from anticipatory guidance: what to expect over weeks, not simply hours.
An indication of a strong program is how they discuss this duration. If management can discuss their comfort-focused procedures, how they coordinate with hospice nurses and assistants, and how they maintain dignity when feeding and hydration become complex, you remain in capable hands.

Where assisted living can still work well
There is a middle area where assisted living, with strong personnel and supportive households, serves somebody with early Alzheimer's very well. If the private recognizes their room, follows meal hints, and accepts tips without distress, the social and physical structure of assisted living can enhance life without the tighter security of memory care.
The warning signs that point towards a specialized program generally cluster: frequent roaming or exit-seeking, night strolling that endangers security, repeated medication rejections or mistakes, or habits that overwhelm generalist personnel. Waiting up until a crisis can make the shift harder. Preparation ahead supplies option and preserves agency.
What households can do best now
You do not have to revamp life to improve it. Small, constant changes make a quantifiable difference.
- Build a simple day-to-day rhythm in the house: very same wake window, meals at similar times, a quick morning walk, and a calm pre-bed routine with low light and soft music.
These practices translate effortlessly into memory care if and when that becomes the ideal step, and they minimize chaos in the meantime.
The core pledge of memory care
At its finest, memory care does not try to restore the past. It builds a present that makes sense for the person you like, one calm cue at a time. It replaces threat with safe freedom, changes isolation with structured connection, and replaces argument with compassion. Families typically tell me that, after the move, they get to be partners or kids once again, not only caregivers. They can visit for coffee and music instead of working out every shower or medication. That shift, by itself, raises quality of life for everyone involved.
Alzheimer's narrows certain paths, however it does not end the possibility of good days. Programs that comprehend the illness, staff appropriately, and form the environment with intent are not just providing care. They are maintaining personhood. And that is the work that matters most.
BeeHive Homes of Hitchcock offers assisted living services
BeeHive Homes of Hitchcock provides memory care services
BeeHive Homes of Hitchcock offers respite care services
BeeHive Homes of Hitchcock provides 24-hour caregiver support
BeeHive Homes of Hitchcock features a small, residential home setting
BeeHive Homes of Hitchcock includes private bedrooms for residents
BeeHive Homes of Hitchcock includes private or semi-private bathrooms
BeeHive Homes of Hitchcock provides medication management and monitoring
BeeHive Homes of Hitchcock serves home-cooked meals prepared daily
BeeHive Homes of Hitchcock accommodates special dietary needs
BeeHive Homes of Hitchcock provides housekeeping services
BeeHive Homes of Hitchcock provides laundry services
BeeHive Homes of Hitchcock offers life enrichment and social activities
BeeHive Homes of Hitchcock supports activities of daily living assistance
BeeHive Homes of Hitchcock promotes a safe and supportive environment
BeeHive Homes of Hitchcock focuses on individualized resident care plans
BeeHive Homes of Hitchcock encourages strong relationships between residents and caregivers
BeeHive Homes of Hitchcock supports aging in place as care needs change
BeeHive Homes of Hitchcock provides a calm and structured environment for memory care residents
BeeHive Homes of Hitchcock delivers compassionate senior and elderly care
BeeHive Homes of Hitchcock has a phone number of (409) 800-4233
BeeHive Homes of Hitchcock has an address of 6714 Delany Rd, Hitchcock, TX 77563
BeeHive Homes of Hitchcock has a website https://beehivehomes.com/locations/Hitchcock/
BeeHive Homes of Hitchcock has Google Maps listing https://maps.app.goo.gl/aMD37ktwXEruaea27
BeeHive Homes of Hitchcock has Facebook page https://www.facebook.com/bhhohitchcock
BeeHive Homes of Hitchcock won Top Assisted Living Homes 2025
BeeHive Homes of Hitchcock earned Best Customer Service Award 2024
BeeHive Homes of Hitchcock placed 1st for Senior Living Communities 2025
People Also Ask about BeeHive Homes of Hitchcock
What is BeeHive Homes of Hitchcock monthly room rate?
The rate depends on the level of care that is needed. We do an initial evaluation for each potential resident to determine the level of care needed. The monthly rate is based on this evaluation. There are no hidden costs or fees
Can residents stay in BeeHive Homes of Hitchcock until the end of their life?
Usually yes. There are exceptions, such as when there are safety issues with the resident, or they need 24 hour skilled nursing services
Does BeeHive Homes of Hitchcock have a nurse on staff?
Yes, we have a nurse on staff at the BeeHive Homes of Hitchcock
What are BeeHive Homes of Hitchcock's visiting hours?
Visiting hours are adjusted to accommodate the families and the resident’s needs… just not too early or too late
Do we have couple’s rooms available at BeeHive Homes of Hitchcock?
Yes, each home has rooms designed to accommodate couples. Please ask about the availability of these rooms
Where is BeeHive Homes of Hitchcock located?
BeeHive Homes of Hitchcock is conveniently located at 6714 Delany Rd, Hitchcock, TX 77563. You can easily find directions on Google Maps or call at (409) 800-4233 Monday through Sunday Open 24 hours
How can I contact BeeHive Homes of Hitchcock?
You can contact BeeHive Homes of Hitchcock by phone at: (409) 800-4233, visit their website at https://beehivehomes.com/locations/Hitchcock, or connect on social media via Facebook
Visiting the Bay Street Park grants peace and fresh air making it a great nearby spot for elderly care residents of BeeHive Homes of Hitchcock to enjoy gentle nature walks or quiet outdoor time.